Press release -
Treating Autoimmune Pancreatitis Without Steroids: Researchers Develop Novel Approach
Osaka [6 June 2023] Researchers identify how activating a protein called aryl hydrocarbon receptor (AhR) protects our body against the development of autoimmune pancreatitis
Autoimmune pancreatitis (AIP) is usually treated with steroids, which may cause severe side effects. Now, researchers from Japan suggest that the selective activation of the transcription factor—aryl hydrocarbon receptor (AhR) - could inhibit the development of AIP with minimal side effects. According to their findings, the binding of AhR to some natural compounds may exert protective effects by increasing the release of pancreatic interleukin-22, as observed in mice and serum from patients with AIP.
Autoimmune pancreatitis (AIP) is a chronic pancreatic disorder that causes inflammation and excessive formation of fibrous connective tissue. It is driven by autoimmunity - a condition in which the immune system mistakenly treats the body's own healthy cells as invaders and attacks them. The clinical management of patients with AIP involves the administration of steroids. However, steroid therapy can cause major side effects including diabetes. There is, thus, a need for AIP treatment alternatives with fewer side effects.
In a new study published on 11 May 2023 in the journal Clinical and Experimental Immunology
(https://academic.oup.com/cei/article/212/3/171/7145827), researchers from Japan have shown that the activation of the aryl hydrocarbon receptor (AhR)—a transcription factor protein that regulates production of immuno-regulatory substances through binding to our DNA—can play a protective role in the development of AIP.
"AhR activation can have a variety of effects on the human body, including changes in metabolism and immunity," says Specially designated Prof. Watanabe from Kindai University, who led the study. "Previous studies, including clinical trials, have shown that the AhR is successful in the treatment of the autoimmune disorder ulcerative colitis (UC) with minimal adverse effects. This made us wonder, 'Could other autoimmune disorders like AIP be treated by activating AhR?'"
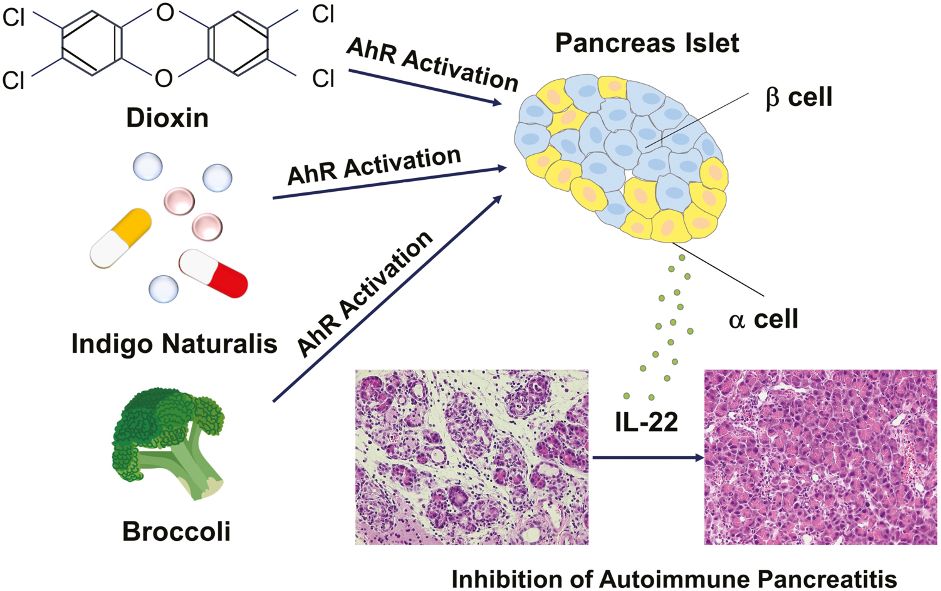
AhR is activated by a variety of binding molecules or 'ligands' that can be natural or synthetic. The natural plant compound Indigo naturalis (IN), for example, is a well-known AhR ligand. In this study, the research team examined how AhR activation affects the development of experimental AIP caused by the activation of plasmacytoid dendritic cells (pDCs) - professional immune cells causing various kinds of autoimmunity. pDCs produce interferon (IFN)-α and interleukin (IL)-33, which are small proteins that mediate immune responses, also known as cytokines.
As a part of this study, the team injected mice with a compound to induce AIP and then provided them with IN and two other therapeutic compounds, indole-3-pyruvic acid (IPA) and 2,3,7,8-tetrachlorodibenzo-para-dioxin (TCDD). Of these, IN and IPA are natural compounds that can be provided through the diet. The researchers found that the activation of AhR by IN, IPA, and TCDD inhibited the development of AIP. They also noticed that these effects were not dependent on the production of the cytokines IFN-α and IL-33.
Their next set of experiments revealed that the interaction of IPA and IN with AhR dramatically increased the production of IL-22 in pancreatic islet α cells. "However, once IL-22 was blocked, the beneficial effects of IPA and IN on the pancreas were completely canceled. These results indicate that AhR activation via IL-22 is crucial for the structure and organization of the pancreas," says Specially designated Pro. Watanabe.
The team then validated their key findings by monitoring serum IL-22 levels in patients with type 1 AIP. As expected, serum IL-22 concentrations were elevated in patients with type 1 AIP whose had reduced symptoms due to the use of the steroid prednisolone—the standard treatment for AIP.
Specially designated Pro. Watanabe concludes by saying, “Overall, our findings suggest that AhR activation via non-steroid compounds such as IPA, IN, and TCDD suppresses the immune responses that characterize AIP by facilitating the production of IL-22 in the pancreatic islet α cells. Our study sheds light on a new therapeutic approach for patients with steroid-resistant autoimmune pancreatitis.”
Reference
Title of original paper: Activation of the aryl hydrocarbon receptor inhibits the development of experimental autoimmune pancreatitis through IL-22-mediated signaling pathways
Journal: Clinical and Experimental Immunology
DOI: 10.1093/cei/uxad040
About Kindai University
Kindai University was established in 1949 after the merger of Osaka Technical College (founded in 1925) and Osaka Science and Engineering University (founded in 1943). Over the past several decades, the university has transformed into a comprehensive educational organization with an ever-growing reputation. Kindai University has over 2,200 full-time faculty members, 6 campuses, and 18 research centers. As an academic institution offering a broad range of programs from across disciplines, Kindai University strives to impart practical education while nurturing intellectual and emotional capabilities. The university’s academic programs are fully accredited by Japan’s Ministry of Education, Culture, Sports, Science and Technology as well as by the National Institution for Academic Degrees and University Evaluation.
Website: https://www.kindai.ac.jp/english/
About Specially designated Professor Tomohiro Watanabe from Kindai University
Dr. Tomohiro Watanabe is a Specially designated Professor at Kindai University’s Department of Medicine/Graduate School of Medical Sciences. He primarily conducts research in the area of gastroenterology, immunology, allergies and connective tissue disease, bacteriology, and molecular biology. He has over 200 research publications to his credit. Specially designated Prof. Watanabe has won several distinguished awards for his exemplary research. He is a well-published book author, and he has also been listed as an inventor on a U.S./WIPO patent discussing the use of muramyl dipeptide in treating inflammation.
Funding information
This study was supported by Grants-in-Aid for Scientific Research (21K15987, 22K07996, and 22K08090) from the Japan Society for the Promotion of Science, Takeda Science Foundation, Smoking Research Foundation, Yakult BioScience Foundation, SENSHIN Medical Research Foundation, and a 2022 Kindai University Research Enhancement Grant (KD2208).
Media contact
Kindai University, Faculty of Medicine and Hospital
General Affairs and Public Relations Division
Release person:Minamikawa
TEL:+81-72-366-0246 (EX3873) FAX:+81-72-365-8300
E-mail:med.koho@itp.kindai.ac.jp



